Patient Education
-
- Achilles Tendonitis
- Ankle Equinus
- Arthritis of Big Toe joint
- Bunion
- Callus
- Capsulitis
- Flatfoot: Acq'd. PTTD
- Ganglion cysts
- Gouty Arthritis
- Hallux Varus
- Hammertoe deformity
- Ingrown toenails
- Kohler’s Osteochondroses
- Limb Length Inequality
- Metatarsal Arthralgia
- Metatarsal Stress Fracture
- Neuroma - Intermetatarsal
- Pediatric Flat Foot
- Peroneal dislocation
- Peroneal tendon tear
- Plantar Fasciitis
- Plantar Fibroma
- Retrocalcaneal Bursitis
- Sesamoid Fracture
- Shin Splints
- Tarsal Tunnel Syndrome
- Tailor's bunion
- Toenail Fungus
- Warts - Verruca Plantaris
-
- Overview
- Diabetic Shoes
- Shoe Modification
- Accommodative Orthotics
- Ankle Foot Orthosis (AFO) - Overview
- Richie Brace® - AFO
- Dorsiflexory Assist Device (Allard® ToeOFF Brace)
- Gauntlet AFO (Arizona®)
-
- Overview
- Preoperative Care
- Day of Surgery
- Postoperative Care
- Bunionectomy
- Bunionectomy - Post-Op
- Neuroma Surgical Care
- No Barefoot Walking
- Activity Limitations
-
-
-
-
-
The Diabetic Foot
Patients with diabetes mellitus have an increased risk of lower extremity ulceration potentially leading to amputation. An “Ulcer” is any injury leading to the loss of the protective skin barrier which can lead to the introduction of bacteria and subsequent infection.
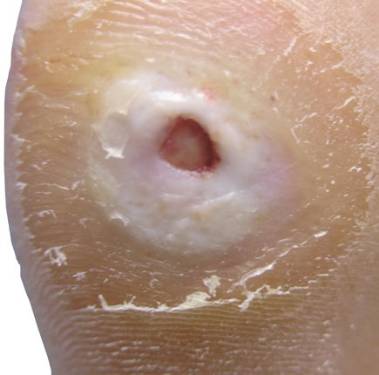 The process of skin injury leading to ulceration, infection and potential amputation is a complex pathway in patients with diabetes mellitus. Diabetic patients over the course of the disease can develop multiple organ system injury related to higher blood sugars over the course of their disease. Elevated blood sugars can cause injury to the eyes, kidneys, vascular system including the heart and peripheral arterial system and the neurologic system leading to loss of sensation. The term “vasculopathy” and “neuropathy” are terms that are generally used to describe “injury” to the vascular and neurologic systems.
The process of skin injury leading to ulceration, infection and potential amputation is a complex pathway in patients with diabetes mellitus. Diabetic patients over the course of the disease can develop multiple organ system injury related to higher blood sugars over the course of their disease. Elevated blood sugars can cause injury to the eyes, kidneys, vascular system including the heart and peripheral arterial system and the neurologic system leading to loss of sensation. The term “vasculopathy” and “neuropathy” are terms that are generally used to describe “injury” to the vascular and neurologic systems.
Neuropathy
For diabetic patients the long term effect on the neurologic and vascular systems plays the most profound influence in the potential development of an ulceration on the foot. By generally accepted processes elevated blood sugars over time can cause injury to the neurologic system. The peripheral nervous system provides your bodies ability to feel pressure, light touch, temperature and even regulate your skins moisture with sweating. The inability to adequately detect light touch pressure for example puts a person at risk for being unable to detect an injury to the foot in a timely manner. For example, if a person is wearing a new shoe that is poorly fitted and walks for a period of time and begins developing a blister, the person who has a complete neurologic response will stop and remove the shoe to relieve the painful shoe. People who have neuropathy may not perceive the pressure stimulus with the shoe and continue walking in the shoe until a significant blister has occurred. A person with neuropathy may not even experience pain as it relates to walking around with a foreign object in their shoe.
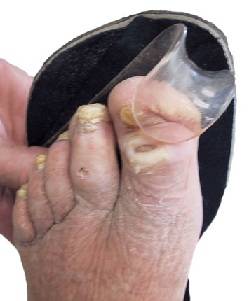 The development of neuropathy can occur very slowly over a number of years and so can be difficult to recognize by someone with diabetes. It has been estimated that 50% of diabetic patients who have had diabetes for twenty years or more will have clinically significant neuropathy. Neuropathy symptoms can include all or some of the following including feelings of burning, tingling, sharp knife like pain, dullness, feeling of swelling to the feet or a feeling of thick leathery skin. The pain associated with neuropathy is usually recognized more at night than during the daytime. Sometimes people who experience neuropathy pain may think that if they have “pain” than they should be able to tell if something is wrong with their feet. Many different types of nerves function to give us our bodies ability to feel completely. Abnormal pressures to the foot may not create a pain response but can develop injury to the skin nonetheless.
The development of neuropathy can occur very slowly over a number of years and so can be difficult to recognize by someone with diabetes. It has been estimated that 50% of diabetic patients who have had diabetes for twenty years or more will have clinically significant neuropathy. Neuropathy symptoms can include all or some of the following including feelings of burning, tingling, sharp knife like pain, dullness, feeling of swelling to the feet or a feeling of thick leathery skin. The pain associated with neuropathy is usually recognized more at night than during the daytime. Sometimes people who experience neuropathy pain may think that if they have “pain” than they should be able to tell if something is wrong with their feet. Many different types of nerves function to give us our bodies ability to feel completely. Abnormal pressures to the foot may not create a pain response but can develop injury to the skin nonetheless.
The ability for patients to feel the pressure of light touch appears to be one of the single most neurologic sensations that have an influence in the development an ulceration.
The use of a nylon monofilament with a 10gm bending force as it is applied to the bottom of the foot at specific areas determines whether there is a loss of sensation to light pressure. The Loss of Protective Sensation (LOPS) with the inability to feel this light touch pressure is an important test.
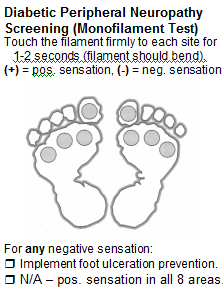 Neuropathy can also effect the portion of the nervous system that controls skin moisture of the feet. Often times diabetic patients with autonomic neuropathy can develop excessively dry skin which can lead to skin cracking and potentially lead to infection.
Neuropathy can also effect the portion of the nervous system that controls skin moisture of the feet. Often times diabetic patients with autonomic neuropathy can develop excessively dry skin which can lead to skin cracking and potentially lead to infection.
Neuropathy can also effect the muscles of the foot with overtime the development of the “intrinsic minus” foot with the atrophy of the small muscles of the foot which can lead to the development of hammertoe deformities.
Treatment of neuropathic pain can be a very difficult challenge. Topical creams that act to counter irritate the skin including the mentholated sports creams can be first used as needed at night. Capsaicin cream which is a derivative of the chili pepper has been shown to be clinically effective in interfering with the pain pathway. Capsaicin can increase the expression of pain over the first few days of use and many times the pain is so marked that patients discontinue it’s use. Many different oral medications are available for use with the effectiveness different between patients. Gabepentin, Lyrica and Cymbalta are commonly used medications that can be very effective in treating the painful symptoms. Physcians often have their own protocols as they approach the difficulty in treating neuropathy symptoms. Managing neuropathy in no way reverses the extent of the neuropathy and only treats the symptoms. Maintaining good blood sugar control is the best long term measure at decreasing the progression of neuropathy.
Peripheral Arterial Disease (PAD)
Peripheral arterial disease (PAD) is another very important potential complication that can occur with diabetes mellitus. The arterial and venous systems are the conduits that transport blood in our body. The arterial vascular system carries oxygen rich blood that is pumped from the heart to be used by the tissues. The venous system transport oxygen depleted blood back to the lungs to be re-oxygenated. Blockage in the arterial vascular system can prevent oxygen rich blood from getting to the tissues including muscles of the legs and feet. Besides Diabetes Mellitus the risk factors for PAD also include high blood pressure and the use of tobacco. Symptoms associated with PAD include the feeling of pain, cramping or fatigue to the calf region while walking. The symptoms generally occur after a predictable amount of walking and often require the suffer to stop and rest prior to resuming the walking activity. These symptoms are termed intermittent claudication. The severity of intermittent claudication is generally determined by the distances in “city blocks” that someone can walk prior to the onset of symptoms. This is a very general way to determine the severity of the PAD but is readily understood by most patients. Patients who have significant neuropathy may however have atypical symptoms of intermittent claudication making a detailed medical history and exam very important. A significant reduction in blood flow to the tissues of the legs and feet can cause pain at rest. “Rest pain” is often times experienced at night when the feet are level with the heart while in bed. The elimination of the pressure associated with a standing position decreases the blood supply getting to the tissues even more and will often times cause calf cramping at night that will awake a person from sleep. The calf pain will be relieved by dangling the legs over the bed or by limited walking around the house. Cramping of the legs at night is very common for many people but if you are able to walk many “city blocks” without intermittent claudication then cramping at night is not “rest pain”
Musculoskeletal Deformity
Abnormal pressures in the diabetic foot can be influenced by underlying bony deformities that are present. The presence of a hammertoe for example can potentially increase pressure and friction on the top surface of the toe that is in contact with the upper material of the toebox.
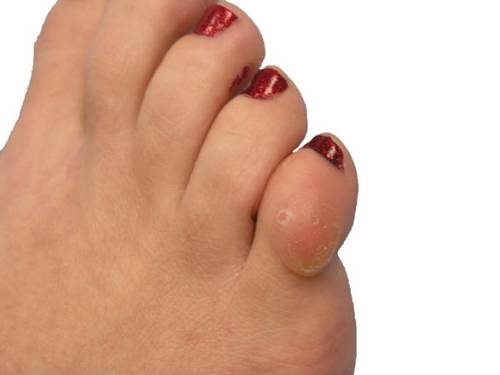 An underlying bunion deformity of the first metatarsal bone may increase pressure and friction on the inside surface of the first metatarsal that contacts the shoe materials. The abnormal pressures and friction over time can lead to the development of a callus which can ultimately lead to the development of an ulceration.
An underlying bunion deformity of the first metatarsal bone may increase pressure and friction on the inside surface of the first metatarsal that contacts the shoe materials. The abnormal pressures and friction over time can lead to the development of a callus which can ultimately lead to the development of an ulceration.
Although surgical correction of underlying deformities may be recommended it is appropriate shoe wear that ultimately can help protect the skin against injury that leads to the development of an open ulcer. Appropriate footwear will often provide the protection the skin needs to prevent ulceration in the region of the bony deformities.
The importance of neuropathy and PAD is that it puts the tissues at greater risk for injury and can increase the risk of infection leading to amputation.
Risk Assessment
Not everyone with Diabetes Mellitus has the same risk of developing an ulceration that could lead to an amputation. A person who has no clinically evident neuropathy or PAD or bony deformity will be a much less risk for developing an ulceration as compared to someone who has clinically significant neuropathy, PAD and a bony deformity. It is important have a comprehensive evaluation to determine if your risk level.
There are several different operating classification systems to help determine the risk of ulceration. These classification systems can at times be confusing because they can appear somewhat complicated. The Lower Extremity Amputation Project (LEAP program) at the Hansen's Disease Center, Carville, Louisiana has established on of the most lasting risk assessment classification systems. The Carville systems main goal is to educate patients to their potential risk for ulceration. change the risk assessment.
Risk Categorization
Category 0: The neurologic exam shows no evidence of loss of protective threshold with the use of the monofilament. There is very little risk of developing foot complications related to the diabetes mellitus. The patient will not need protective shoewear.
Category 1: There is evidence of loss of protective threshold but no noted foot deformity or previous history of open ulceration. This patient is unable to feel the monofilament in two out of five locations tested on the bottom of the foot. These patients due to their inability to feel the monofilament light touch pressure may not be able to recognize a skin injury if it occurs. Patients should make sure they do not walk barefoot. Patients in this category may be Medicare qualified for diabetic based shoe and insert if there is evidence of preulceration callous but can also typically wear a wide toe box style shoe like an athletic shoe.
Category 2: Loss of protective sensation is noted and is present with deformity without history of ulceration. This patient will need Medicare approved diabetic extra depth shoe with inserts or custom accommodative orthotics to accommodate the deformity and protect the foot from injury
Category 3: This patient has a history of foot ulceration. Loss of protective threshold is present. This patient will need Medicare approved diabetic shoe or custom shoe with custom insole after complete healing of the foot ulceration.
Patients who have document peripheral arterial disease will be elevated to the next Risk Classification number
More resources at Diabetes.org
Suggested Forms
-
Most people with diabetes can prevent any serious foot problem by following these simple guidelines.
Schedule an Appointment

Please call 805.543.7788 for San Luis Obispo, 805.434.2009 for Templeton, or email us to request an appointment.

